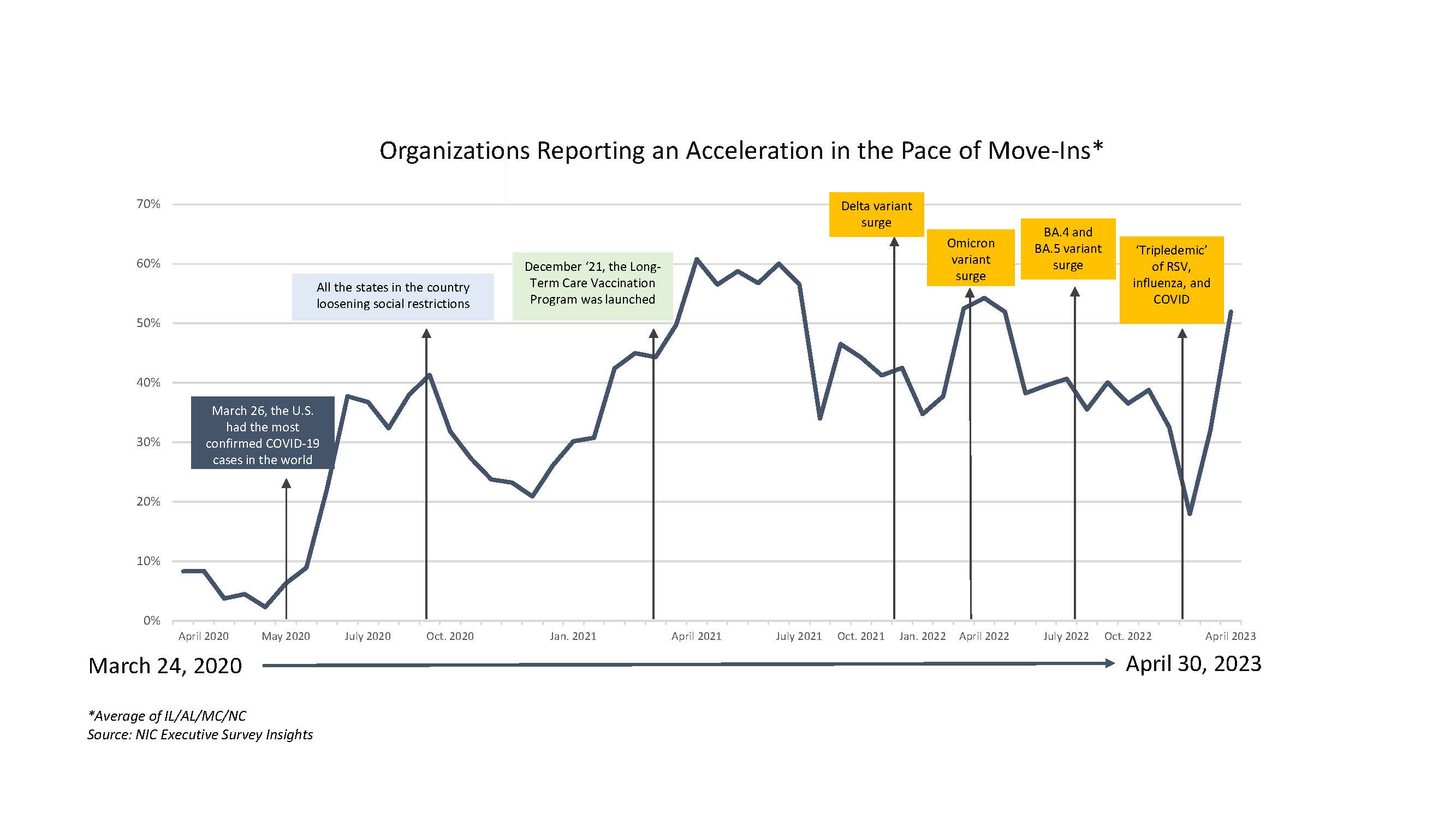
“When aggregated across all care segments, one-half of responding operators (52%) report an acceleration in the pace of move-ins in April 2023. This marks the highest level of operators reporting an acceleration since April 2022, when 54% of organizations reported the pace of move-ins to be accelerating. However, this is still below the peaks experienced from April to July 2021, when approximately 60% of operators reported an acceleration in the pace of move-ins.
The higher cost of debt is having an influence on organizations’ development pipeline. More than one-half of independent living operators (57%) report the higher cost of debt is having a significant impact to their development pipeline, followed by one-half of memory care (50%) and assisted living (49%) operators. Just under one-third of nursing care operators (29%) report the higher cost of debt having a significant impact on their development pipeline.”
–Ryan Brooks, Senior Principal, NIC
This ESI survey includes responses from April 1, 2023, to April 30, 2023, from owners and executives of 45 small, medium, and large senior housing and skilled nursing operators across the nation, representing hundreds of buildings and thousands of units across respondents’ portfolios of properties. The number of properties owned or operated by survey respondents in the April 2023 ESI ranges from one to as many as 400. More detailed reports for each “wave” of the survey and a PDF of the report charts can be found on the NIC COVID-19 Resource Center webpage under Executive Survey Insights. 
In the April 2023 ESI, the share of operators reporting an acceleration in the pace of move-ins in the past 30 days has increased across all care segments. More than one-half of assisted living (56%), memory care (56%), and independent living (52%) operators report an acceleration in the pace of move-ins. For independent living operators, this marks the third consecutive month with an increase, up from 37% in March 2023 and from 27% in February 2023. Slightly fewer than one-half of nursing care operators (44%) report acceleration in the pace of move-ins, up from 28% the previous month.
When aggregated across all care segments, approximately one-half (52%) of operators report an acceleration in the pace of move-ins in April 2023. This marks the highest level of operators reporting an increase since April 2022, when 54% of organizations reported an increase. However, this is still below the peaks experienced from April to July 2021, when approximately 60% of operators reported an acceleration in the pace of move-ins.
 The increasing proportion of organizations reporting an acceleration in the pace of move-ins is creating optimism with regard to the anticipated timeframe for occupancy to recover to pre-pandemic (March 2020) levels. Across all care segments, almost two-fifths of operators (38%) anticipate occupancy to recover in 2023, while one-quarter (25%) anticipate the recovery won’t occur until 2024. Only 6% of operators anticipate it will take until 2025 or later for occupancy to recover.
The increasing proportion of organizations reporting an acceleration in the pace of move-ins is creating optimism with regard to the anticipated timeframe for occupancy to recover to pre-pandemic (March 2020) levels. Across all care segments, almost two-fifths of operators (38%) anticipate occupancy to recover in 2023, while one-quarter (25%) anticipate the recovery won’t occur until 2024. Only 6% of operators anticipate it will take until 2025 or later for occupancy to recover.
Perhaps predictably, the needs-based settings are the most optimistic about the occupancy recovery timeline, with almost one-half of nursing care (46%) and two-fifths of assisted living (41%) and memory care (40%) operators anticipating occupancy recovery in this calendar year. Conversely, for the wants-based setting of independent living, only one-quarter of operators anticipate occupancy to recover to pre-pandemic levels in 2023.
Despite optimistic occupancy recovery timelines, difficulties persist on the labor front. Attracting community and caregiving staff is cited as the biggest challenge by respondents (78%), followed by rising operator expenses (76%) and staff turnover (67%). The proportion of organizations reporting more than 25% of full-time, open positions across their organization has more than doubled – to 12% — since the last time this question was asked in November and December 2022, when only 5% of organizations reported more than 25% of full-time positions as open.
These openings are a leading cause of operators experiencing a staffing shortage and greater than 90% of operators report experiencing a staffing shortage in April 2023. Among these operators, just under one-tenth (8%) indicate the shortage to be severe. Three-quarters (75%) of respondents indicate their staffing shortage to be moderate, followed by one-sixth (17%) who indicate the shortage to be minimal.
Agency staff is still being used to supplement job roles, with nurse aides (38%) and nurses (33%) being the roles that are most often being supplemented. Food services employees (13%) and plant operations employees (10%) follow as the next most likely job roles to be supplemented by agency staff.
Even with the open, full-time positions being high in April 2023 and attracting community and caregiving staff being cited as the biggest challenge, almost one-half (48%) of operators believe staffing challenges will improve in 2023, followed by one-quarter (28%) of operators who anticipate seeing improvements in 2024, and the remaining one-quarter not anticipating seeing improvements until 2025 or later.
New questions to the ESI survey ask about the impact of the current operational environment (occupancy rates, operating expenses, inflation, etc.) on the ability to service debt as well as the impact of the higher cost of debt on their organization’s development pipeline.
 With regards to the impact of the current operational environment on the ability to service debt, half (50%) of nursing care operators reported there was no impact, followed by just under one-half of assisted living (46%), independent living (43%), and memory care operators (41%). Comparatively, just under one quarter of nursing care operators (23%) reported the current environment had a significant impact on their ability to service debt, while one-sixth of memory care operators (17%), and one-tenth of independent living (11%) and assisted living operators (10%) reported a significant impact.
With regards to the impact of the current operational environment on the ability to service debt, half (50%) of nursing care operators reported there was no impact, followed by just under one-half of assisted living (46%), independent living (43%), and memory care operators (41%). Comparatively, just under one quarter of nursing care operators (23%) reported the current environment had a significant impact on their ability to service debt, while one-sixth of memory care operators (17%), and one-tenth of independent living (11%) and assisted living operators (10%) reported a significant impact.
 While most respondents indicate the current operational environment is having no impact to their ability to service debt, the higher cost of debt is having an influence on organizations’ development pipeline. More than one-half of independent living operators (57%) report the higher cost of debt is having a significant impact to their development pipeline, followed by one-half of memory care (50%) and assisted living (49%) operators. Just under one-third of nursing care operators (29%) report the higher cost of debt having a significant impact on their development pipeline.
While most respondents indicate the current operational environment is having no impact to their ability to service debt, the higher cost of debt is having an influence on organizations’ development pipeline. More than one-half of independent living operators (57%) report the higher cost of debt is having a significant impact to their development pipeline, followed by one-half of memory care (50%) and assisted living (49%) operators. Just under one-third of nursing care operators (29%) report the higher cost of debt having a significant impact on their development pipeline.
Despite the impact of higher debt costs, two-fifths of operators are still considering diversifying their product offerings in 2023. Among organizations who are considering product diversification, three-quarters plan to diversify into lower acuity settings (76%), while only one-sixth plan to diversify into higher acuity settings (18%). A small portion of responding organizations (6%) plan to expand into both lower and higher acuity settings.
April 2023 Survey Demographics
- Responses were collected between April 1 and April 30, 2023, from owners and executives of 45 senior housing and skilled nursing operators across the nation.
- Owners/operators with 1 to 10 properties comprise roughly one-half of the sample (56%). Operators with 11 to 25 properties and operators with 26 properties or more account each account for roughly one-quarter (22%) of respondents.
- More than one-half of respondents are exclusively for-profit providers (58%), one-third operate not-for-profit seniors housing and care properties (33%), and 9% operate both.
- Many respondents in the sample report operating combinations of property types. Across their entire portfolios of properties, three-quarters (71%) of the organizations operate seniors housing properties (IL, AL, MC), 22% operate nursing care properties, and 36% operate CCRCs – also known as life plan communities.
The May 2023 ESI survey is currently open and will be collecting responses through May 31, 2023. If you are an owner or C-suite executive of seniors housing and care and would like an invitation to participate in the survey, please contact Ryan Brooks at rbrooks@nic.org to be added to the list of recipients.
NIC wishes to extend a heartfelt thank you to the owners and operators who have contributed to this survey over the past three years. It is remarkable that we have now completed more than 50 waves of surveys. We have surveyed through numerous challenges — COVID-19, threats of a looming recession, labor shortages, inflation, and rising expenses — many of which still persist. As we continue to navigate through these challenges, your input and real-time insights help ensure the narrative on the senior housing and care sector is accurate. By demonstrating transparency, you build trust. Thank you.
